From Energy Savings to Infection Prevention: Why SDCV Matters for NHS Resilience

The National Health Service (NHS) supports millions of lives every single day. But today, the system is under unprecedented pressure. With patient numbers soaring, energy prices volatile, and infection control at the top of the post-pandemic agenda, the “old way” of managing hospital buildings is no longer enough.
To withstand these challenges, the service needs more than just hard-working staff; it needs NHS Resilience.
What does a “Resilient NHS” look like?
True resilience is the ability of a hospital to provide safe, high-quality care even during a crisis or a surge in demand. While we often focus on beds and medicine, one of the most critical factors in a hospital’s defense is invisible: the air.
Smart Demand-Controlled Ventilation (SDCV) is emerging as a game-changer for healthcare estates. By using intelligent, sensor-driven technology, SDCV actively reduces infection risks, slashes energy waste, and protects the very people who keep the NHS running.
The Growing Challenges for NHS Capacity
The NHS is currently facing many pressures, making it more important than ever to strengthen healthcare systems and ensure reliable, efficient hospital operations.
Hospitals must treat more patients while also keeping healthcare workers safe.
The vicious cycle of Infection Prevention:
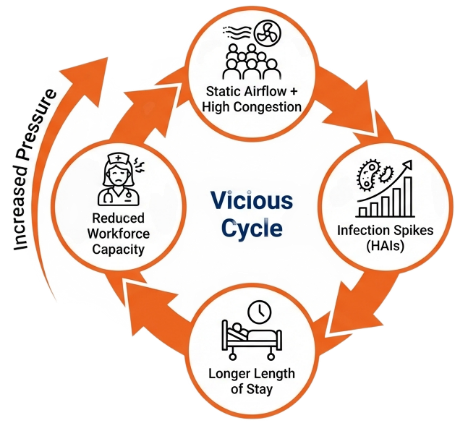
Poor ventilation and overcrowded spaces allow airborne pathogens to build up, driving spikes in healthcare-associated infections (HAIs). As infections rise, patient stays lengthen and staff absences increase, reducing workforce capacity and putting further pressure on already stretched facilities. This creates a self-reinforcing cycle where constrained airflow and system strain continue to amplify infection risk and operational inefficiency.
Rising Patient Demand
Hospitals across the UK are seeing more patients every year.
According to NHS England, waiting lists for treatment have increased in recent years due to high demand and pandemic delays, with the waiting list for hospital treatment rising to nearly 7.8 million in September 2023; since then, it has fallen by around 5%, but it still remains higher than pre-pandemic levels.
This creates pressure on hospitals.
Some reasons for rising patient numbers include:
- Growing population
- Aging population
- Long waiting lists
- More chronic diseases
These challenges affect hospitals because they must treat more patients with limited resources.
Workforce Pressure in Hospitals
Doctors, nurses, and healthcare staff work very hard to support patients. However, many hospitals face workforce shortages. According to The King’s Fund, the NHS has faced staffing shortages in many roles, including nurses and general practitioners.
Some common workforce challenges include:
- Long working hours
- High patient numbers
- Stress and burnout
- HAI (Hospital Acquired Infections) among nurses and staff
Creating safer hospital environments helps protect healthcare workers and improve overall healthcare system stability.
The NHS Net Zero Commitment
Another challenge for the NHS is environmental sustainability. Hospitals and trust buildings use large amounts of electricity and gas heating.
According to NHS England’s Greener NHS programme, the NHS aims to become the world’s first net-zero national health service in response to the growing threat that climate change poses to public health and healthcare delivery.
In October 2020, the NHS became the first health system globally to commit to reaching net zero carbon emissions, setting out a clear strategy called Delivering a Net Zero Health Service.
The programme sets two main net zero targets against a 1990 baseline:
- Net zero by 2040 for the emissions the NHS directly controls (the NHS Carbon Footprint), with an interim goal of an 80% reduction by 2028-2032.
- Net zero by 2045 for the emissions the NHS can influence (the NHS Carbon Footprint Plus), with an 80% reduction ambition by 2036-2039.
This commitment involves reducing carbon from buildings, travel, medicines, supply chains, and care models, and mobilising the NHS’s workforce of around 1.3 million staff to drive change.
The target is:
| Target | Year |
| Net zero emissions from NHS operations | 2040 |
| Net zero emissions from the supply chain | 2045 |
Reducing energy demand is critical to both lowering costs and building a more resilient NHS—creating an opportunity to improve efficiency without compromising patient safety or care quality.
Why Air Quality Matters for Healthcare Efficiency
Hospitals are often defined by clinical excellence – people, medicine, and technology. Yet one of the most critical drivers of outcomes and efficiency is often overlooked: Air Quality.
Clean, well-managed air protects patients and staff, reduces risk, and enables safer, more efficient care delivery at scale.
The Ventilation Gap in Hospitals
Many hospital buildings were built decades ago. Older ventilation systems may not meet modern healthcare standards.
Insufficient or excess ventilation can lead to several problems:
- Spread of airborne diseases
- Poor indoor air quality
- Uncomfortable environments
- High building operating costs
According to healthcare research on hospital ventilation, poor airflow can increase infection risk in hospitals.
Airborne Infection Risks
Hospitals treat patients with many different illnesses. Sometimes infections spread inside hospitals. These are called hospital-acquired infections (HAIs).
According to the UK Health Security Agency, infections can spread through air, surfaces, and close contact.
Poor ventilation increases the risk of airborne transmission. Cleaner air helps reduce infection spread and create safer healthcare environments.
Infection Prevention and Hospital-Acquired Infections in NHS Hospitals
Preventing infections is one of the most important goals in healthcare. Hospitals use many methods to reduce infection risk.
Impact of Hospital-Acquired Infections
Hospital infections can create serious problems. They affect patients, hospitals, and healthcare workers.
According to Proxximos, Hospital Acquired Infections (HAIs) cost the NHS an estimated £2.7 billion annually and are associated with around 28,500 patient deaths each year.
According to research published in healthcare studies, hospital infections increase healthcare costs and patient recovery time.
Here are some common impacts:
| Problem | Effect |
| Longer hospital stay | Patients take longer to recover |
| Higher treatment costs | Hospitals spend more resources |
| Increased health risks | Some infections can be dangerous |
How Smart Ventilation Improves Healthcare Systems
Advanced ventilation systems do more than just move air; they transform hospitals into safer, more efficient environments. SDCV (Smart Demand-Controlled Ventilation) provides a multi-layered defense for the healthcare system.
Mitigating Infection Risks
In high-traffic areas like waiting rooms, emergency departments, and open wards, airborne pathogens can linger. Traditional systems often run at a flat rate, regardless of how many people are in the room.
In contrast, SDCV uses real-time sensors (monitoring CO2 and particulate matter (PM), TVOC levels) to detect when a space is crowded. It automatically boosts airflow to flush out contaminants when risk is highest. This proactive approach significantly lowers the chance of hospital-acquired infections (HAIs), keeping the clinical environment stable.
Protecting Healthcare Workers
The backbone of the NHS is its people. Healthcare staff who spend 12 hours shifts in poorly ventilated spaces are at higher risk of illness and fatigue.
By maintaining optimal Indoor Air Quality (IAQ), SDCV:
- Reduces staff sick days by limiting the spread of seasonal viruses.
- Improves cognitive function by maintaining correct Occupant comfort levels.
- Boosts morale by providing a demonstrably safer workplace.
Elevating – Patient Safety and Recovery
For vulnerable hospital patients, the air they breathe in is vital. Smart ventilation ensures a constant supply of purified air that:
- Minimize secondary airborne infections
- Regulate temperature and humidity for better patient comfort
- Support faster discharge rates through faster recovery
By integrating these smart technologies, trusts can move away from reactive maintenance and toward a robust, future-proof infrastructure that protects everyone under its roof.
Energy Efficiency and NHS Resilience
Hospitals use large amounts of energy every day. Heating, cooling, lighting, and ventilation systems run continuously to maintain safe clinical environments. This makes hospitals some of the most energy-intensive buildings in the public sector.
Improving energy efficiency helps healthcare facilities reduce operating costs while maintaining safe indoor environments for patients and staff.
Energy Savings with Smart Ventilation
Traditional ventilation systems operate at a fixed rate regardless of occupancy or air quality. This often means heating or cooling empty spaces and using more electricity than necessary.
Smart Demand Controlled Ventilation (SDCV) adjusts airflow based on real-time conditions such as occupancy and air quality. This allows hospitals to maintain healthy indoor air while using significantly less energy.
Research presented in healthcare ventilation studies shows that smart ventilation systems can:
- Reduce energy use by more than 40% through system optimization
- Use up to 9× less energy per cubic metre of air compared with traditional HVAC systems
- Improve airflow efficiency while maintaining infection control standards
These improvements allow hospitals to maintain safer environments while reducing unnecessary energy consumption.
Supporting the NHS Net Zero Plan
The NHS England has committed to reducing carbon emissions through its Greener NHS Programme, which aims to achieve a net zero health service by 2040.
Reducing energy use in hospital buildings is a key part of this strategy. Energy-efficient ventilation systems help healthcare facilities lower emissions, reduce energy costs, and support long-term sustainability goals.
By combining smart ventilation technology with energy optimization, hospitals can create healthier indoor environments while contributing to national environmental targets.
Improving Hospital Efficiency
Hospitals must treat many patients every day. Better systems help improve hospital efficiency and capacity.
Faster Room Preparation
After a patient leaves a room, cleaning and air quality restoration are required. SDCV ventilation systems can reduce room turnaround time by 250-300%, enabling hospitals to prepare rooms faster.
Benefits include:
- Faster room availability
- More patients are treated daily
- Reduced waiting times
This ensures hospitals can handle higher patient volumes efficiently.
Better Patient Flow
Efficient hospitals manage patient movement smoothly, reducing bottlenecks.
Advantages include:
- Shorter waiting times
- Faster treatment
- Better patient experience
By improving room turnover and patient flow, hospitals can treat more patients safely while maintaining high standards of care.
The Future of NHS Resilience
Healthcare technology continues to improve. Hospitals are adopting smarter systems to improve safety and efficiency.
Future hospitals may include:
- Smart ventilation technology
- Real-time monitoring systems
- Energy-efficient infrastructure
- Data-driven healthcare decisions
Conclusion
The NHS sits at the intersection of rising demand, workforce pressure, infection risk, and ambitious net zero targets. Addressing these challenges in isolation is no longer enough.
Air quality is the missing link that connects them all.
By rethinking ventilation through intelligent, demand-controlled systems, hospitals can simultaneously reduce infection risk, improve staff wellbeing, unlock capacity, and cut energy consumption.
This is the shift—from reactive infrastructure to proactive resilience.
Rensair’s Smart Demand-Controlled Ventilation (SDCV) enables NHS trusts to move beyond compliance and cost-saving, toward a future where buildings actively support clinical outcomes, operational efficiency, and sustainability goals. Get in touch to know more about our technology.
Because a truly resilient NHS is not just about treating more patients—
it’s about creating environments where patients recover faster, staff perform at their best, and systems adapt in real time.
Rensair will be attending key healthcare and infection prevention events in 2026, including:
If you’re attending, let’s connect.
We’d welcome the opportunity to discuss how NHS trusts can strengthen Infection Prevention & Control, reduce operational strain, and build long-term resilience through smarter ventilation.
